|
| |
Pancreatitis and its
complications
by Dr.Mir Mustafa
Health Page|
Diseases and Remedies |
Articles
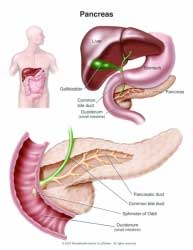
What is the function of the pancreas?
The pancreas is an organ responsible for the
production of significant hormones, such as the insulin, glucagons, and somatostatin. It is also an exocrine gland that is responsible for secreting
pancreatic juice, which contains digestive enzymes that pass to the small
intestine. These enzymes aid in further breakdown of carbohydrates, proteins,
and fats in the chime, the partially digested mass of food that is forced into
the small intestines.
Note: Glucagon is an important hormone involved in carbohydrate metabolism and
somatostatin is a hormone produced in the hypothalamus (portion of brain) that
inhibits the release of somatotropin (growth hormone) and other hormones.
Exocrine glands produce secretions for the surface of organs like the mammary
glands, sweat glands and saliva glands.
Note: The pancreas is a large gland organ in the digestive and endocrine system
of vertebrates. It is located behind the stomach and close to the duodenum — the
first part of the small intestines.
What causes pancreatitis?
Pancreatitis is mainly caused by: Alcoholism, gallstones, abdominal surgery,
certain medications, cigarette smoking, cystic fibrosis (an inherited chronic
disease that affects the lungs and digestive system); endoscopic retrograde
cholangiopancreatography (ERCP), when used to treat gallstones; Family history
of pancreatitis, high calcium levels in the blood (hypercalcemia), high levels
of parathyroid hormone in the blood (hyperparathyroidism), high triglyceride
levels in the blood (a condition in which triglyceride levels are elevated),
infections, injury to the abdomen, pancreatic cancer and ulcer.
What are the symptoms of pancreatitis?
The signs and symptoms of pancreatitis may vary depending on the type of
ailment. However, in acute pancreatitis the signs include:
Upper abdominal pain, abdominal pain that radiates to the back, abdominal pain
that is triggered after eating or even before attempting to eat, nausea or
vomiting, fever, mild jaundice and rapid pulse, tenderness in the stomach.
The signs of chronic pancreatitis include: Upper abdominal pain, indigestion,
weight loss, and oily, smelly stools.
What complications are relevant with pancreatitis?
 Pancreatitis
can cause serious complications such as: Breathing difficulty, diabetes, kidney
failure, malnutrition. Pancreatic cancer and several other infections Pancreatitis
can cause serious complications such as: Breathing difficulty, diabetes, kidney
failure, malnutrition. Pancreatic cancer and several other infections
What tests are relevant for diagnosing pancreatitis?
Tests may include: Blood tests to examine the complete blood count (CBC) and the
Lipase and Amylase, the digestive enzymes made by the pancreas; computerised
tomography (CT) scan; abdominal ultrasound; endoscopic ultrasound; magnetic
resonance imaging (MRI)
When can a person seek medical care?
In most cases, the pain and nausea associated with pancreatitis are severe
enough for a person to seek medical attention because of the associated
complications such as: Inability to take medications or to drink and eat because
of nausea or vomiting; Severe pain that is not relieved by the counter pain
relief drugs; difficulty in breathing; pain accompanied by fever or chills,
persistent vomiting, weakness and exhaustion. Pain can also be felt in the
presence of other medical conditions such as pregnancy.
Is pancreatitis preventable?
In all cases, pancreatitis cannot be prevented. But, to help reduce the risk of
developing the ailment, it is advisable to reduce consumption of alcohol, avoid
smoking and eat a healthy diet that is low in fat and to maintain a normal body
weight according to the guidelines of the Body Mass Index.
What are the other treatment options?
Treatment depends on the causes and severity of the condition. In acute
pancreatitis treatment involves: hospital care, intensive care in hospital;
fasting and intravenous fluids until the inflammation of the pancreas improves,
endoscopy — a thin tube is inserted through the oesophagus to enable the doctor
to examine the pancreas. Surgery in presence of gallstones to remove the
gallbladder to aid against further attacks.
However, in rare cases, surgery is considerably necessary to remove damaged or
dead parts of the pancreas. Lifestyle modification by eliminating alcohol.
In chronic pancreatitis it is advisable to: Reduce or avoid fat intake;
supplement digestion with pancreatic enzyme tablets when having food; get rid of
alcohol; insulin injections, if the endocrine function of the pancreas is
compromised; pain relief drugs.
by Dr.Mir Mustafa
Dr.Mir Mustafa
|
|
( Courtesy:
http://main.omanobserver.om )
| |
|



 Pancreatitis
can cause serious complications such as: Breathing difficulty, diabetes, kidney
failure, malnutrition. Pancreatic cancer and several other infections
Pancreatitis
can cause serious complications such as: Breathing difficulty, diabetes, kidney
failure, malnutrition. Pancreatic cancer and several other infections Dr.Mir Mustafa
Dr.Mir Mustafa