|
| |
Information:
Kidney stones
Main
Article page |
Beauty articles
|
Health page |
Computers|
Diseases |
Education |
Entertainment |
Family
Business |Fitness|
Fruits and Vegetables
|
Jobs |
General |
Personality|
Technology
|
Tourism |
Useful Tips
General Knowledge |
Biography Page|
Heroes & Incredible peoples
|
Inventions
Health Page|
Diseases and Remedies |
Articles|
List of diseases
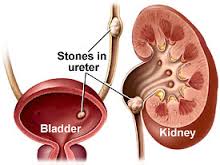
Kidney stones usually comprised of a compound called calcium
oxalate, are the result of an accumulation of dissolved minerals on the inner
lining of the kidneys. These deposits can grow to the size of a golf ball while
maintaining a sharp, crystalline structure.
The kidney stones may be small and pass unnoticed out of the
urinary tract, but they may also cause extreme pain upon exiting.
Kidney stones that remain inside the body can lead to many
conditions, including severe pain and ureter (the tube connecting the kidney and
bladder) blockage that obstructs the path urine uses to leave the body.
www.KidneyStoners.org: 1. What is a kidney
stone?
Kidney stones are the formation of crystalline structures in the urinary tract
(which includes the kidneys, ureters, and bladder). These stones can cause pain,
infection, and kidney damage. Stones can be small, from 1 mm to very large,
filling up an entire kidney. For pictures of stones, see our stone gallery.
2. Do I have a kidney stone?
For patients experiencing their first stone episode, the pain can be so severe
and sudden that it stops them in their tracks. Without prior knowledge of what a
stone episode feels like, it can be confusing and frightening to go through this
amount of discomfort, which is usually described as the worst pain someone has
ever experienced. A trip to the emergency room is usually required to make the
diagnosis and provide treatment for an active kidney stone. X-rays, usually a CT
scan, can be used to confirm that a stone is present.
3. What are the symptoms of passing a kidney stone?
Stone pain is often described as stabbing and extremely severe. Women commonly
say that it is worst than having a child. The pain can start in the upper back
(flank) and then migrate to the abdomen and groin. Changing positions does not
help relieve the pain. The pain of a kidney stone is primarily due to blockage
of the urine drainage coming down the small tube called the “ureter” that
connects a kidney to the bladder. See a diagram of the urinary system.
It is thought that the increased pressure stretches the kidney and ureter,
causing the pain. This is why stone pain can come and go in waves, as the
drainage tube is periodically blocked by the stone trying to make its way out.
As the stone moves further down the tube, the pain experienced moves down the
body. Other symptoms common during a stone episode include seeing blood in the
urine, nausea & vomiting, and feeling the urge to urinate. Once a stone is
passed and makes it way out of the ureter tube and into the bladder, most
patients describe a sensation of instant relief as the blockage and pressure is
relieved. However, stones can take from days to weeks to pass. See a diagram of
locations where stones typically get obstructed.
Continued down....
4. Do all kidney stones cause pain?
Most doctors feel that kidney stones only cause pain if they are blocking the
ureter and trying to pass down towards the bladder. Stones that are not
obstructing, such as those located in the kidney’s calyxes, are generally
thought to be non-painful. This explains why some patients can have extremely
large stones filling up their entire kidney with no or minimal pain.
However, it does appear that some non-obstructing stones can cause pain because
of either blockage of small tubular structures in the kidney itself (the
collecting tubules) or for other unclear reasons. Supporting this view is a
recent medical journal article suggesting that the treatment of small
non-obstructing “papillary” stones may provide pain relief. (Gdor et al,
Multi-institutional assessment of ureteroscopic laser papillotomy for chronic
pain associated with papillary calcifications, J Urol 2011) Additionally,
testimonials from many kidney stone patients (including a urologist with a
personal history of kidney stones) suggest that some non-obstructing stones can
cause pain.
5. What causes a kidney stone?
Kidney stones affect 1 out of 10 people during their lifetimes. They are more
common than most people realize. There are many factors that determines whether
someone will develop a stone with some being under a person’s control while
others are out of their hands.
Common factors influencing kidney stone development:
Gender: Men are two to three times more likely to form stones
Race: Caucasians have the highest stone rates as compared to other races
Age: Stones occur most commonly between the 20s to 50s
Geography: Those living in hot dry environments are at increased risk.
Additionally, those living in the Southeastern United States appear to be at
particularly increased risk of forming stones.
Seasonal climate: Stone development is more common during the summer months due
to dehydration from higher summertime temperatures and possibly also from higher
concentrations of calcium in urine resulting from increased sun exposure which
can lead to higher levels of Vit D production.
Occupation: Those working in jobs with exposure to climate and dehydration are
more prone to stone development.
Body weight: There are higher rates of stones in those with increased weight and
body mass index.
Genetics and medical conditions: Individuals with a history of some conditions,
such as medullary sponge kidney or renal tubular acidosis are prone to forming
stones. Those with a personal family history of stones may have two to three
times increased risk of forming stones.
Infections: Chronic urinary tract infections can lead to the development of
infection related stones, known as struvite stones.
6. Can I take something to dissolve my kidney stone?
Patients often ask whether something can be taken to dissolve their stones.
Unfortunately, the most common stone types (calcium oxalate and calcium
phosphate, accounting for 80% of all stones) cannot be dissolved with
medications.
However, in patients with uric acid stones, which account for 5-7% of stones,
medication (potassium citrate) can be successfully given to dissolve the stones,
helping them to pass and preventing them from re-developing.
Patients with the less common cystine type stones (1-3% of stone formers) can
also benefit from potassium citrate and water intake to help dissolve their
stones. Cystine stone formers additionally can be treated with D-penicillamine
or α-mercaptopropionylglycine to help bind and dissolve their stones.
Finally, patients with struvite, or “infection”, stones were in the past more
commonly treated with hemiacidrin irrigation solution which is dripped directly
onto stones through a tube placed directly into the kidney. However, because of
potentially serious side effects from this medication and the difficulty in
giving it, this type of therapy is now uncommon.
Learn more about different types of stones.
7. How do kidney stones form?
There are many factors that lead to the development of kidney stones. For
details and a visual time-line of the steps in stone formation, see: How do
stones form?
8. Was it something I ate/drank?
In most patients, we find diet is not the main reason that caused a stone to
form in the first place. Other important factors also play a role in determining
whether someone is “prone” to forming stones. In other words, a non-stone-former
can eat the exact same diet as a stone-former and never get stones.
That said, diet can play an important role in the prevention of future stones.
The three most important dietary factors for most stone formers to modify in
reducing their risk of future stones are to increase total fluid intake,
decrease sodium intake, and and decrease protein (meat) intake.
Some commonly held beliefs of foods that promote stones including cola, tea,
coffee, and calcium intake have not been shown to be true. In fact, research
suggests that increasing tea, coffee, and calcium intake can actually reduce
stone risk, while cola does not appear to have a significant effect (Curhan et
al, Am J of Epidemiology, 1996). See more on kidney stones myths.
9. Can I prevent another kidney stone?
Yes!, there are many effective ways to help prevent another stone. Basic dietary
changes can reduce your chances of forming another stone by half while more
involved medical treatment can reduce that even further. While these changes may
not guarantee that you will not form another stone, they can make it less likely
that you will have to experience another painful stone episode. See our stone
prevention center to find out more.
10. What are my treatment options for my kidney stone?
Treatment options for stones include allowing a stone to pass by itself, using
medications to help pass a stone, and surgery to treat or remove a stone. Our
stone treatment center has more information, including videos and diagrams of
stone surgeries to help you better understand your options.
11. What are the signs of a kidney stone emergency?
If you think you are passing a stone, signs indicating that you should seek
immediate medical attention include:
Fever above 101.5 degrees Fahrenheit
Other symptoms of a urinary tract infection with a stone, including burning
during urination, cloudy urine, or bad smelling urine
Persistent nausea and vomiting
Intolerable pain
Certain medical conditions can make passing a stone potentially more dangerous,
including those with only one kidney, those with diabetes, or those with
decreased kidney function
12. How long does it take to form a kidney stone?
It appears that stones can form in as short a period of time as three months.
This is based on research of soldiers deploying to Kuwait and Iraq where the
mean time to development of a symptomatic stone was 93 days in the hot desert
environment. (Evans and Costabile, J Urol, 2005)
13. What is my risk of forming another kidney stone?
In general, the chances of developing another stone is about 40-50% over five
years. In other words, 1 out of 2 new stone formers should expect to develop
another stone within the next five years. However, there are many effective ways
to reduce the chances of recurrence with simple diet changes. See our prevention
center for more details.
14. Am I going to be able to pass my (insert size here) stone?
Your likelihood of passing a stone will primarily depend on its size, its
location, and how long you have been trying to pass a stone. We go over this in
our infographic available here: What are my chances of successfully passing
passing my stone?
15. What surgery option should I choose?
There are three common surgeries for stones. These include ureteroscopy,
shockwave lithotripsy, and percutaneous nephrolithotripsy. We go over the pros
and cons of each here: How do I choose which surgery to have for my kidney
stones?
16. What is a ureteral stent?
A stent is a flexible hollow tube placed inside the ureter. It allows urine to
drain around a stone and helps the ureter heal after surgery. It is entirely
inside your body and is not visible from the outside. Stents can cause you to
feel like you have to urinate often, can cause minor bleeding, and can cause
pain. Find out more about stents here: All about ureteral stents.
17. How is a ureteral stent placed?
Ureteral stents are usually placed in the operating room by your doctor. A
flexible wire is slid up the ureter and the stent is slid over the wire. The
wire is removed and the stent remains. At each end of the stent are natural
“curls” to keep it in place until it is removed or exchanged. See more about
stent placement here: How is a ureteral stent placed?
18. How is a stent removed?
Ureteral stents can be removed in two ways. Most commonly, your doctor will
remove the stent by placing a camera into your bladder through your urethra (the
tube where urine exits your body). The stent is grasped with an instrument and
removed. The second method is used when a string is left attached to the stent.
The string, which is visible exiting the urethra, is pulled until the stent
comes out. See more about stent removal here: How is a ureteral stent removed?
19. Why do I have pain after my stent was removed?
Some mild amount of discomfort after stent removal is expected. However, in some
patients, severe pain may occur for several hours after stent removal. This is
thought to be due to spasms of the ureter or swelling and temporary blockage
developing after the stent comes out. Not enough is known about this phenomenon
but one recent study suggests it may occur in as many as half of patients. In
the study, a single dose of a non-steroidal anti-inflammatory drug given 15
minutes before stent removal was highly effective at preventing the severe pain
from developing. You can read more about the study here: Severe pain after stent
removal: How often does it occur and can anything prevent it?
( Courtesy: KidneyStoners.org is a
non-commercial website that was started to help patients better understand their
condition and the options available for treatment and prevention. For more
information visit
http://www.kidneystoners.org )
More information about Kidney stone
See kidney stone pictures
| |
|



